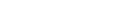Africa has made incredible improvements immunising children against preventable diseases such as polio, pneumonia, diphtheria, measles and tuberculosis. By 2014, 77% of the continent’s children were immunised. Compared to 1980, when only 5% of African children were vaccinated, this is a drastic improvement.
Despite these achievements, the immunisation agenda in Africa remains unfinished. Large numbers of children are still not vaccinated and die from vaccine-preventable diseases. In 2013, more than three million children under the age of five suffered this fate.
And of the 19 million children worldwide who did not receive the required three doses of diphtheria-tetanus-pertussis vaccines, more than 40% – or more than 7.6 million – of these children were from sub-Saharan Africa.
The origins of immunisation
Immunisation is important – it protects people against diseases by vaccinating them.
Annually, immunisation prevents more than three million deaths globally from measles, diphtheria, tetanus, and whooping cough. It also prevents millions of children from being permanently disabled by polio or tuberculous meningitis.
Immunisation became a public health intervention across the globe in 1974 after smallpox was successfully eradicated by immunising people. As a result of the success, the World Health Organisation initiated the Expanded Programme on Immunisation. The organisation recommended six vaccines. These were against tuberculosis, diphtheria, tetanus, pertussis (whooping cough), polio, and measles.
In the last four decades, there has been extraordinary progress in improving vaccination coverage. The 72% increase in sub-Saharan Africa’s children receiving three doses of diphtheria-tetanus-pertussis vaccines shows how well this global immunisation programme has worked with the general health system.
There has also been significant progress to expand the schedule in Africa. Once finalised, it should include new vaccines against eight or more diseases. Gavi, the global vaccine alliance, has played a key role in these vaccine introductions.
Immunisation successes
Aside from the turnaround in diphtheria-tetanus-pertussis vaccines, there has also been huge success against meningitis and polio. Both are evidence of the strides national immunisation programmes have taken in Africa.
In the 1990s, devastating meningitis epidemics occurred every year in the African meningitis belt, which stretches from Senegal to Ethiopia. In 1997, there were 250,000 cases and more than 25,000 deaths. This led African leaders to call for a vaccine to be developed to eliminate group A meningococcus – a predominant cause of epidemic meningitis.
The Meningitis Vaccine Project, a collaboration between the World Health Organisation and PATH (an international nonprofit organisation), then developed an affordable, tailor-made vaccine. When the vaccine was introduced in mass campaigns in 2010 it had a dramatic impact, breaking the cycle of the epidemics.
Before vaccine development came into play, nearly half a million people were paralysed annually as a result of polio. But community leaders and armies of community workers got involved and transformed polio eradication in Africa. The continent has not had a case of wild poliovirus for more than one year – a momentous achievement.
Immunisation programmes like these have had a great impact on child deaths. In 2000, 9.9 million children died globally before their fifth birthday. By 2013, this decreased to 6.3 million, with 3.6 million less pneumonia-, diarrhoea- and measles-related deaths.
Sub-Saharan Africa contributed half of the under-five deaths worldwide in 2013. The main causes of these deaths were pneumonia, diarrhoea, preterm birth complications, and malaria. Africa has a child population of about 389 million.
Pneumonia is the single largest infectious cause of child deaths worldwide, killing almost one million children under five in 2013. It accounts for 15% of all child deaths. Vaccination is the best way to prevent pneumonia.
Africa lags behind
Immunisation has the potential to do more than it already has.
The global health community has collectively recognised the potential of immunisation, and established the Global Vaccine Action Plan. The plan envisions a world without people dying from vaccine-preventable diseases.
But Africa has dropped the ball. One of its targets was to vaccinate at least 90% of children across the continent with three doses of diphtheria-tetanus-pertussis vaccines by the end of 2015.
Only 38% of African countries achieved this by last year. More than 60% of the children who did not receive these vaccines are from ten countries. Of these, five are in sub-Saharan Africa – the Democratic Republic of Congo, Ethiopia, Nigeria, Uganda, and South Africa.
There are several challenges around vaccinations that have resulted in these countries not meeting the targets. These include:
-
insufficient public awareness of the benefits of vaccination;
-
lack of trust in health systems;
-
inadequate human resources and access to care;
-
untimely vaccinations and service delivery;
-
deficient infrastructure; and
-
poor-quality data.
External evaluations have identified several inconsistencies in the immunisation data collected in Africa. Good quality data is essential to create appropriate programmes that can be put into action. Without knowing who has been vaccinated against which diseases, it is difficult to undertake evidence-informed corrective actions to improve immunisation programmes.
Hold leaders accountable
African countries must critically assess their position and develop evidence-informed interventions to overcome the challenges around vaccination.
The Global Vaccine Action Plan provides general approaches to meet targets. But it needs complementary tactics from African countries, along with robust monitoring and accountability frameworks, if mass immunisation is to succeed.
African leaders should be held accountable to meet the country targets they agreed to, and to honour their international commitments.
![]()
Written by Charles Wiysonge, Professor of Clinical Epidemiology at the Faculty of Medicine and Health Sciences, Stellenbosch University
This article was originally published on The Conversation. Read the original article.
EMAIL THIS ARTICLE SAVE THIS ARTICLE
To subscribe email subscriptions@creamermedia.co.za or click here
To advertise email advertising@creamermedia.co.za or click here